Picture this: A bustling insurance claims department where professionals grapple with laborious, time-consuming manual processes, never-ending volumes of paperwork, long claims triaging and processing times, soaring operational costs, claims processing inaccuracies that translate to overpayments, and delays that impact customer satisfaction. The insurance sector has been looking towards technology to fast-track claims processes, thereby driving the customer experience.
With advancements in artificial intelligence (AI) and new-age automation, achieving human-like intelligence and unparalleled efficiency is gradually becoming a reality. When integrated into insurance claims management software, these technologies can revolutionize claims processing. In this blog, we will uncover the journey from manual to effortless claims and explore the role of AI and automation in claims processing.
Table of Contents
The Future of Insurance Claims Processing
The Promise of AI and Automation in Revolutionizing Claims Processing
How AI Processes Faster and More Fairly
How to Successfully Implement AI and Automation in Claims Processing
The Future of Insurance Claims Processing
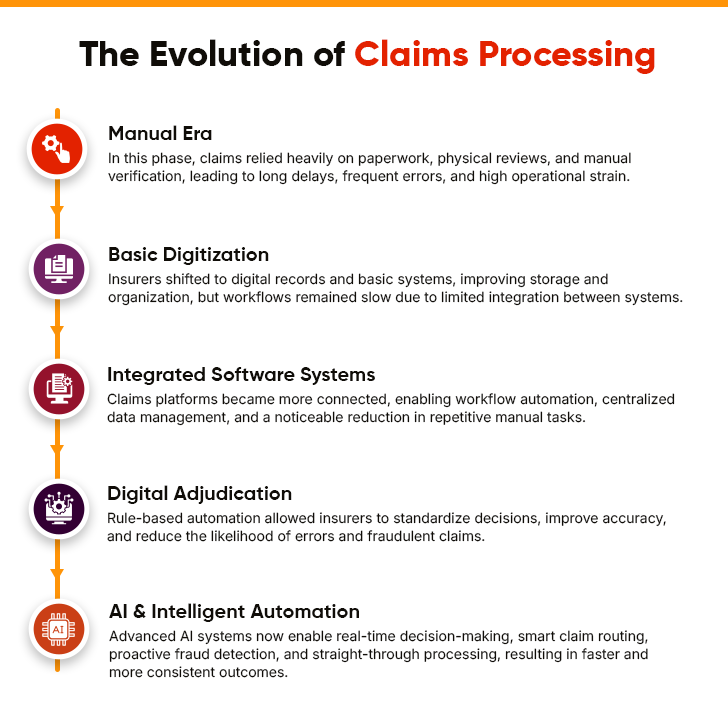
Insurance claims processes have undergone a massive overhaul driven by technological advancements and industry trends. Historically, these processes were paper-heavy. However, they have now been transformed by AI-driven claims management automation solutions. Let’s explore the evolution of the claims management process:
1. The Era of Manual Processing
Traditionally, claims management relied heavily on manual methods. It involved paperwork, in-person reviews, face-to-face meetings, and telephonic conversations. While the process was typically straightforward, it proved inefficient, resulting in delays. Mistakes and errors would seep in as claim adjusters manually assessed each claim.
2. The Advent of Basic Digital Tools
The introduction of computers and basic digital tools marked a significant shift in the claims management landscape. This era witnessed insurance businesses move from paper-based filing systems to digital records and data management systems. While this made things more organized and efficient, these early insurance claims processing systems had limitations. For instance, these systems couldn’t seamlessly integrate with other systems and workflows.
3. Software Advancements and Integration
With technological advancements, insurance claims management software has evolved into more sophisticated systems. These advanced solutions facilitated seamless data integration, storage, and retrieval. Full-featured claims management software emerged during this period, capable of handling intricate tasks such as document management and workflow automation. This significantly reduced manual labor and enhanced overall efficiency.
4. The Evolution of Digital Claims Processing
A crucial milestone in the evolution was the shift toward fully digital claims processing. Digital adjudication systems automated numerous steps in the process, resulting in smoother operations, improved claim decision accuracy, and reduced error and fraudulent claim rates.
5. The Rise of Automation
Automation in claims processing revolutionized routine tasks by automating mundane activities. Insurance claims process automation allowed human resources to redirect their focus toward more challenging and strategic tasks. This fostered improved productivity, employee satisfaction, speed, and accuracy. This led to Straight Through Processing (STP) of claims, opening a new dimension for reducing the claims ratio and enhancing the customer experience.
6. Integration of AI in Insurance Claims
The integration of AI and machine learning in insurance claims management paved the way for a transformative shift. These technologies automate complex tasks such as assessments, intelligent document processing, fraud detection, and customer interactions. AI could handle data effectively, resulting in faster claims resolutions and improved customer satisfaction.
Transform Your Claims Process with Automation
The Promise of AI and Automation in Revolutionizing Claims Processing
“Cloud is the enabler; data is the driver, and AI is the differentiator”
– Julie Sweet, CEO, Accenture
AI and automation are no longer experimental technologies in insurance claims. They are becoming essential tools for insurers looking to improve speed, accuracy, and operational control in an increasingly competitive market. Here’s how AI-enabled insurance claims automation benefits insurers:
I. Convenient Claims Reporting
Insurance claims process automation has transformed claims registration, making it simpler, more convenient, and more accessible. The traditional claims filing process can seem complex, and the complex forms can leave policyholders frustrated.
However, the claims process is automated using AI-driven technologies to make the claims registration experience smoother. For instance, in the event of an accident, AI chatbots can guide users through the next steps, collect required information, and initiate the claims process. This not only improves efficiency but also accuracy. In fact, McKinsey estimates that AI can improve claims accuracy by 3-5 percent.
II. Automated Data Management
The role of AI in insurance claims extends beyond mere claims reporting. It streamlines both data entry and analysis. For one, AI-powered insurance claims management software can automatically extract data from structured and unstructured documents such as invoices, forms, receipts, and more, thereby minimizing human intervention.
Not only does it ensure data accuracy and completion, but it also significantly speeds up claims processing. AI-based claims software can also deep-dive into data to unlock meaningful insights and flag suspicious behavior. This helps insurers proactively navigate fraud detection. Lastly, insurers can use the insights obtained from these systems to adjust their policies and premiums.
III. Enhanced Customer Experience
The success of any insurance business is closely linked to the experiences it offers to its customers. The claims experience directly impacts the policyholder’s decision to stay with the insurer. Leveraging AI and automation in claims processing helps insurance businesses deliver a better claims experience, driven by personalization, convenience, and proactive communication throughout the entire claims lifecycle. AI in insurance claims can help anticipate queries and offer instant solutions. On the other hand, insurance claims process automation enables real-time updates, allowing customers to track their claim status and other developments.
IV. Stronger Fraud Detection and Risk Control
By implementing AI in claims processing, insurance companies can detect fraud with greater accuracy and efficiency than by using conventional methods. Through machine learning, models can examine both past and present data across a variety of claims to unearth changes or inconsistencies that might indicate fraudulent activity. Insurers can thus identify potentially fraudulent claims at an early stage, thereby avoiding unnecessary disbursements, reducing losses, and, safeguarding the interests of genuine policyholders against the surge in premium rates.
In fact, the deployment of AI in fraud detection has substantially reduced the number of false claims, and human skills have been redirected to areas where they are most necessary. As such, Deloitte estimates that property and casualty insurers could potentially save up to US$160 billion by 2032 by adopting AI-powered, real-time fraud detection and analytics.
V. Better Support and Communication for Policyholders
Automating insurance claims processing keeps policyholders well informed at every step of their claims process. Examples of AI-powered initiatives designed to enhance the policyholder experience include chatbots and virtual assistants. They not only can offer uninterrupted support services by being available round the clock, but also can answer the most common questions, provide step-by-step instructions for filling out the form, and even keep policyholders informed about the status of the claim via real-time updates.
This steady, anticipatory mode of communication reduces customers’ reliance on calling support teams and increases their satisfaction. By implementing personalized, honest communication, insurance companies build client trust and thereby strengthen their relationships with policyholders.
How AI Processes Faster and More Fairly
One of the most powerful ways AI and automation are changing claims processing is by dramatically speeding up the time it takes to decide and pay claims. Traditionally, insurers could take days or even weeks to settle straightforward claims because human adjusters had to review every form, photo, and document manually.
Now, with intelligent systems in place, basic claims can be resolved in minutes or even seconds.
Take a look at this example featuring a top-tier US-based property insurance adjusting company that employed artificial intelligence to automate the evaluation of property damage using state-of-the-art deep learning models for image analysis.
The insurance company was stuck with inaccurate loss estimation reports for a long time because surveyors frequently confused roof material types, shingles, and structural features; as a result, quality checks had to be repeated, slowing settlement.
An AI model based on machine learning and computer vision was implemented to continuously monitor roof damage photos, determine the type of shingles and roofing structures, and correlate these findings with loss report matrices.
Our system integration with the insurer’s existing software not only helped eliminate human errors and bottlenecks but also significantly accelerated the processing of claim loss reports and enhanced service delivery to carriers. Claim teams enjoyed increased efficiency, turned work around faster, and were given a blueprint for full automation of their operations.
All in all, AI speeds up claims handling in a few practical ways:
- Instant Data Capture: Natural Language Processing (NLP) can read and extract key details from documents, such as insurance forms, emails, and invoices, without anyone manually entering information. This means no lost or incorrectly entered data and a much faster start to the claim review.
- Smart Routing of Work: When a claim is first submitted, AI can assess how complex it is and decide whether it can be fully handled automatically or if it needs a human expert’s attention. This ensures simple claims move through swiftly while the right specialists get complex cases.
- Automated Damage Evaluation: For auto or property claims, AI can analyze photos submitted by policyholders. Imagine submitting images of car damage from your phone. The system measures the extent of damage and suggests repair costs in minutes, something that once took hours of manual assessment.
Beyond speed, AI also improves fairness and consistency. Machines don’t fatigue, overlook details, or interpret rules differently from one day to the next. This reduces the risk of mistakes that can delay claims or frustrate customers. When systems consistently follow the same rules, outcomes are closer to what policyholders expect, and disputes over decisions are less common.
How to Fix the Information Gap in Healthcare Claims Management with AI
How to Successfully Implement AI and Automation in Claims Processing
Adopting AI is not about installing new software. It is about redesigning how claims move across the organization. Insurers that see real results treat automation as operational transformation, not just a technology upgrade.
Here is what practical implementation looks like:
1. Map the Current Claims Journey
It is advisable to first delineate how a claim moves through the system without automation.
Think about these questions:
- Where does it take the most time?
- Where does the same information get input again?
- Where are the errors mostly happening?
Quite a few insurance companies reveal that the greatest delays occur at the stages of document intake, running validation checks, and getting approvals from within. Typically, these are the areas where automated claims processing solutions can significantly increase efficiency right from the start. If this mapping is not done, automation is merely an addition to broken workflows rather than a repair.
2. Segment Claims Intelligently
It is impractical to fully automate every claim. Therefore, a clear segmentation model is more effective:
- Low-value, rule-based claims can be completely automated
- Mid-level claims can be sent for AI-assisted review
- Complex or high-risk claims need human decisions supported by AI
Employing AI for claims processing in a hybrid manner achieves harmony. AI can verify coverage, extract policy details, cross-check documents, and calculate estimated payouts. The human adjusters are then free to work on those cases that involve disputes, are out of the ordinary, or require sensitive decisions. This way, operational risk is reduced while the turnaround time improves.
3. Strengthen Data Before Scaling
AI is really about data quality. Legacy systems can still be very inconsistent; different departments have different claim categories, there are duplicate records, and the documentation is not always structured.
Before scaling automation:
- Clean historical claims data.
- Standardize formats across departments
- Define clear documentation requirements
- Remove duplicate or incomplete records
Strong data governance ensures more reliable decision-making while also reducing false fraud alerts. Skipping this step means that even the most advanced automation systems will give out results that are not trustworthy.
4. Start with a Controlled Pilot
A pilot approach builds internal confidence and provides measurable proof before expanding investment. Hence, don’t go for a big launch right away. Instead:
- Choose one line of business
- Select one claim type
- Run a time-bound pilot
- Compare results against manual benchmarks
Measure impact through:
- Average settlement time
- Error reduction
- Rework rate
- Customer satisfaction
5. Redefine Workforce Roles
Automation inevitably changes teamwork processes, but it doesn’t take away the expertise.
Claims adjusters are freed from manual data entry so they can focus on handling exceptions and complex cases. Managers move from supervising paperwork to monitoring dashboards and fraud indicators. Explaining these changes clearly helps to reduce resistance and pave the way for a smooth adoption.
6. Build Governance and Oversight
Governance ensures automated decisions remain explainable and fair. This protects both the insurer and the policyholder.
Automated processes have to be transparent and compliant. Set up:
- Audit trails for automated decisions
- Escalation triggers for unusual claims
- Periodic model performance reviews
- Compliance checkpoints
Conclusion
Historically, insurance businesses have often avoided large-scale technology adoption in claims management, preferring to rely on the acumen and accuracy of their claims managers. However, owing to factors such as growing customer expectations, the rise of insurtech, and evolving business models, insurance businesses are now investing in technologies like AI and automation. Given the advantages of leveraging automation and AI in insurance claims, it becomes evident that these technologies are paving the way for the future of the industry.